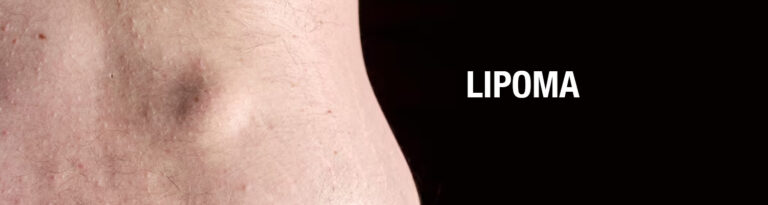
Have you observed a plate-shaped, elastic structure under your skin that moves with pressure? Ulcer, oncocytoma, and other conditions that happen subcutaneously may have left you with a lipoma. So, what is a lipoma weighed down, and why should you be aware of this common yet not too well-understood problem?
Lipoma Definition:
A lipoma is a non-malignant tumor made of three different cells that create fatty tissue and grow underneath the skin. These blunders are often identified by their tender squish rubber appearance and are usually painless. Such nodules and lumps are often mobile and occur on the skin, the distinguishing symbol of other types of tumors and growths.
Lipomas usually have a slow-growing course with the numbness and discomfort normally occurring when they reach a size large enough to be detected. These are benign tumors that one can live with, but they can still be annoying or aesthetically displeasing. Examples are: if they appear in areas that are too visible or tactile such as the face, neck, arms, or torso.
Prevalence of Lipoma:
The understanding of the prevalence of lipomas means how common the condition is within a specific community. It is the indicator that shows the number of people who suffer from lipomas at a given time. The degree of lipoma occurrence varies by region and the age and gender composition of the population. However, the general notion is that lipomas are quite common within the global population. They are observed with good frequency in clinical settings, with some estimates placing their prevalence at about 1% in the population. Lipomas can be found in persons of any age and race, as well as gender, but they are most diagnosed in adults between the ages of 40 and 60.
Risk Factors for Lipoma:
Risk factors of lipomas recognize specific factors or situations that may raise an individual’s probability of developing these benign tumors.
Family History:
People whose families have lipomas tend to be more likely to develop them as well, thus showing a genetic disposition. Epigenetic variability within families may be one of the shared genetic factors contributing to lipoma development, although the exact genes are often poorly understood. It is the case that having parents or siblings, who have a history of lipoma increases your chances of developing one
Age:
Lipomas occurring in middle-aged and elderly adults are observed more frequently. The risk goes up with age. Lipomas can occur at any age, but they are more frequently found among individuals over 40 years old. Precisely, what causes lipoma to occur with increasing incidence with age is not well understood, but it might be due to alterations in fat metabolism, tissue structure, or conditions associated with aging.
Gender:
Lipomas are just slightly more common in men than women, though they can arise in both genders. Factors that may contribute to the gender disparity in the prevalence of lipomas are not entirely known and could be related to hormonal, genetic, or environmental factors. The trunk and upper body are the most common sites of lipomas for men, and the arms and thighs are the most common sites of lipomas for women.
Obesity:
Animal studies have found a relationship between obesity and lipoma development. This may be because of increased adipose tissue. Obesity is described as a collection of adipose tissue throughout the body and the accumulation of fat mass may lead to the development of lipomas which makes obesity more likely. However, although not all lipomas are associated with obesity, lean individuals can also have these bumps on the body.
Certain Genetic Conditions:
Some genetically related syndromes or conditions, such as familial multiple lipomatosis, do increase the risk of developing lipomas. These conditions are associated with a high tendency for the existence of several lipomas over the body. To be more specific, familial multiple lipomatosis is an inherited condition that causes the formation of lipomas all over the body, which usually start to form in early adulthood.
Hormonal Factors:
Hormonal imbalances or alterations may increase the risk of lipoma emergence most significantly during the states of pregnancy or menopause. Changes in hormone levels, like during pregnancy or hormonal treatment, may alter fat metabolism and distribution, therefore, it is possible that lipomas will develop because of it. Lipoma formation in some patients may additionally be affected by hormonal changes in menopause which is associated with menopause.
Previous Trauma or Injury:
In the case where fat is affected by trauma or injury, the probability of developing lipomas in the affected area may rise, but it is still not fully understood at this point whether there is a simple causal relationship between them. This theory suggests that trauma could be the reason for abnormal growth or proliferation of the fat tissue, which could result in lipoma formation. Still, more studies should be done to illuminate the exact association between trauma and lipoma creation.
Certain Medications:
In fact, the use of any particular drug(s) such as corticosteroids has been linked to the risk of lipoma formation. Steroids are a therapeutic agent mankind has used for a variety of medical conditions, yet it is linked to changing how fat is metabolized and where it is stored, thus they become the link to lipomas’ appearance. Nevertheless, there is no sufficient proof that corticosteroid use increases one’s chances of getting a lipoma, and further research must be carried out.
The awareness of the prevalence as well as risk factors for lipoma counts as the first and foremost condition. It supports the identification of those who are most likely to suffer from this disease and the development of prevention and management strategies.
Types of Lipoma:
Lipoma can take a variety of forms, which have some specific traits and importance. Let’s examine each one of them, in order to make it clearer.
1) Conventional Lipoma:
This is the most common type of lipoma, and its soft, movable qualities under the skin make it highly distinguishable. Although conventional lipomas usually occur slowly and do not hurt, they are regarded as benign. They can be located anywhere on the body but the most commonly found locations are on the arms, thighs, abdomen, and neck.
2) Superficial Subcutaneous Lipoma:
Just as the lipomas are ordinarily found in the body, superficial subcutaneous lipomas are found just under the skin. They are typically seen as small, smooth bumps which can occur in places such as the neck, shoulders, back, or arms.
3) Deep Lipoma:
When one gets older deep-filled lipomas develop within the body most often in the muscle or around organs. Although deep lipomas are not as common as their counterpart lipomas, they can grow in size before they are noticed because they’re located in the deeper part of the body. They may present as firm masses and at times can cause discomfort or impingement/impingement on the neighboring structures.
4) Intramuscular Lipoma:
The name gives a hint that intramuscular lipomas develop within the muscle tissue. Since they are in the fiber of muscles, these lipomas are usually difficult to diagnose. These may be felt as relatively firm and rubbery areas and often painful or may cause restricted movement if they compress nerves or blood vessels within the musculature.
5) Angiolipoma:
Angiolipoma is a lump containing both fatty tissues and blood vessels. Angiolipomas are different as they may be painful or tender to touch. Other lipomas are not like that. They may appear as diffuse, multiple lesions and can be on the arms, legs, or trunk.
6) Spindle Cell Lipoma:
Spindle cell lipomas are a less frequent subtype of lipoma, described by their great time lag in growth and unique spindle-shaped cells. They are usually fatty tumors and appear soft, spongy, and oval on the back, shoulder, or neck. The behavior of a spindle cell lipoma is mostly benign but in rare cases the lipoma may recur after surgical removal.
7) Pleomorphic Lipoma:
The pleomorphic lipoma is rare, like the other subtype of lipoma, frequently found in the neck or shoulders. They are defined by their specific cellular morphology and may be encountered as unstructured, irregular tumors that are large in size. Although in general harmless, the risk of recurrence of pleomorphic type is higher than that of other lipoma types in particular.
Knowing the types of lipomas is able to be helpful in out of the mystify of these benign growths. If you find any lumps in your body that are unfamiliar to you, you should call on a doctor to perform a proper diagnostic and that will ensure reassurance.
Causes of Lipoma:
Lipoma has undefined causes sometimes. Nevertheless, they are believed to be the product of fat cells’ proliferation. Some factors such as genetic predisposition, hormones, and slight injuries to the affected areas can be the cause of the development of bone disease.
Genetic Predisposition:
The family connection is the most determinant in the occurrence of lipomas. People with a family history of lipomas are more prone to develop them and that seems to point to a role of genetics in lipoma development.
Adipocyte Proliferation:
Lipomas originate from the enlargement of adipocytes, the cells that store fat within the body. While the mechanisms behind the initiation of multiple, these factors’ role and impact are not fully understood but may entail genetic, hormonal, or environmental factors.
Hormonal Imbalance:
There is a possibility that fluctuations of the hormones, for example, estrogen and progesterone, may cause lipoma. Hormonal variations that occur during the process of puberty, pregnancy, or menopause could result in an increase in the growth and differentiation of the adipocytes.
Trauma or Injury:
Although not a direct cause, trauma or injury to fatty tissues may initiate the formation of lipomas among these susceptible persons. Breakdown of normal growth of adipocytes upon trauma may result in lipoma formation in the affected region due to the disruption.
The causes and risk factors can be understood and triggers can be identified so that a person can do a lot to prevent lipomas through proactive measures.
Symptoms of Lipoma:
In most cases, lipomas are not symptomatic except for the presence of a soft, moveable lump below the skin.
Soft, Movable Lump:
Typically, lipomas are found as soft, rubbery lumps just beneath the skin. They move when touched and they can be palpated like a small ball that is located beneath the skin surface. The texture can be described as doughy or squishy, making it different from other types of skin growth.
Slow Growth:
Lipomas have a unique attribute of growing slowly over time. Frequently, they begin as tiny, hardly noticeable nodules that steadily grow bigger and bigger for weeks, months, or even years. Sometimes lipomas stay small and do not show any symptoms, but others can grow and become more prominent or bothersome.
Location:
Lipomas can develop in any part of the body where there is an accumulation of fat cells. The most often visited sites include the neck, shoulders, back, arms, abdomen, or thighs. Nevertheless, lipomas can occur in the less common sites such as the scalp, hands, feet, and internal organs. Sometimes the area where the lipoma is located affects whether it makes the person feel any symptoms or discomfort, especially if it compresses nearby nerves or tissues.
Discomfort or Pain:
Even though lipomas usually do not give pain, larger or deeper lipomas may cause discomfort or mild pain, which may be felt if they compress nearby structures such as nerves or muscles. This uneasiness may be realized as aching, soreness, or a feeling of pressure in that specific part. There are few situations where lipomas situated in sensitive areas may cause more serious discomfort or limit movement.
Changes in Appearance:
The size and location of lipomas determine the visible deformation in the shape of the skin. Small lipomas may be just tiny bumps or lumps under the skin’s surface, but larger lipomas may look like bulges or deformities in the area in which they are located. In such a case the surrounding skin may look stretched or dimpled especially if the lipoma grew rapidly or attained massive size.
Rare Symptoms:
In extraordinary situations, lipomas can be associated with tenderness, inflammation, and rapid growth. The presence of soreness or tenderness around the lumpy area may indicate inflammation or irritation of the tissues surrounding the papules. Any besides normal size and shape of lipomas should be investigated immediately by a healthcare professional to exclude complications and financial conditions.
Cosmetic Concerns:
Lipoma being in a highly visible area or in a prominent part of the body may cause cosmetic concerns, particularly, if an individual loses self-esteem or develops issues of body image. Lipomas do not usually represent any danger to the health and do not need to be surgically removed, still, some people want them to be hence removed for purely aesthetic conclusions, to eliminate local discomfort or inconvenience.
While many lipomas are tiny, painless, and not noticed you should know this. But when you feel or see such things as new lumps or skin changes, it’s advisable to make an appointment with a healthcare provider.
Complications of Lipoma:
Although lipomas are usually not dangerous and, generally, harmless, they sometimes can lead to complications and, (occasionally), could cause problems depending on their size, location, and individual circumstances. Some potential complications and risks include:
Discomfort and Pain:
Larger or deeper lipomas may be just uncomfortable or even cause mild pain when they interfere with the adjacent nerves, muscles, or organs. These nuisances can be experienced as aching, tenderness, or a dull pain in the area that is affected by them.
Affecting Movement:
Lipomas near joints or muscles can affect movement, as they cause a limitation in a range of motion and may present stiffness or difficulty in doing basic things. In certain instances, individuals could experience weakness or muscle imbalance as a result of a lipoma presence.
Nerve Compression:
In certain cases, lipomas which are relatively large can press on adjacent nerves and thus cause symptoms such as pain, tingling, numbness or weakness in the area they are related to. Nerve compression can disturb sensory and this may even impair performance in the affected portion of the body.
Organ Compression:
Lipomas located inside or in close proximity to organs may cause pressure on the surrounding structures thus leading to complications such as gastrointestinal symptoms, urinary troubles, or respiratory complaints. In severe cases, lipoma can cause compromising of organs, which requires medical treatment to ease the symptoms and prevent other complications.
Cosmetic Concerns:
It is cosmetically concerning in locations of the body where the lipomas are readily visible or prominent, especially if these distort the person’s normal appearance and self-esteem. Whilst cosmetic issues do not constitute health hazards in themselves, their effect on one’s quality of life and psychological well-being is of great concern.
Rare Complications:
A malignant transformation is an ultra-rare event for lipomas; liposarcomas arise from swellings of fat cells that are cancerous. However, the possibility of malignant transformation, however small, brings into perspective the need for thorough evaluation and close surveillance of these lipomas, especially when there is any evidence of rapid growth, atypical symptoms, or change in appearance.
Nevertheless, although lipomas rarely have complications, patients should be aware of the risk factors of these benign tumors because most of the time they are discovered accidentally. Consideration of a healthcare professional to obtain the correct diagnosis, evaluation, and management is necessary, at least the lipoma causes some symptoms or concerns.
Diagnosis of Lipoma:
Lipomas are normally diagnosed with a straightforward process of examining the area and characterizing it.
Physical Examination:
A healthcare provider will perform a full body checkup and pay attention to the specified area(s) where there may be lumps or nodules. A lipoma is usually palpable as it feels like a soft, rubbery, and somewhat moveable structure underneath the skin. The healthcare provider will examine the lipoma(s) regarding the size, location, and texture during the examination.
Medical History:
The detailed medical history of the person, such as symptoms that are associated with the lipoma, family history of similar growths, or any trauma or injury to the affected area helps in finding out the diagnosis and the management of the condition.
Imaging Tests:
In some instances, diagnostic imaging tests like ultrasound or MRI (magnetic resonance imaging) may be prescribed to verify the diagnosis of a lipoma, especially if the mass is deep-lying or if the nature of the growth is vague. These imaging modalities can enable the sight of the size, location, and characteristics of the lipoma which will be helpful in treatment planning and choosing the surgical extent where needed.
Biopsy (Optional):
Although biopsy (surgical removal of a tissue sample is being done for examination under a microscope) is not usually needed for the diagnosing of a lipoma, it may be done in some situations to exclude other conditions or if there are worries about the nature of the growth. Nevertheless, in most cases, lipomas are diagnosed by clinical examination and imaging criteria.
Follow-Up:
Upon the diagnosis of a lipoma, healthcare professionals recommend regular check-ups for the size of the lesion, especially if it is asymptomatic and not cause any major concerns. If the lipoma becomes suspicious by the manifestation of abnormal features such as rapid growth, changes in appearance, or symptoms such as pain or discomfort, further examination and treatment may be required.
Overall, the diagnosis of a lipoma is most of the time straightforward and can be attained with the help of physical examination, medical history, and diagnostic imaging. Early detection and the right diagnosis are critical for determining the right treatment plan to help produce the best results for people living with lipomas.
Treatment of Lipoma:
Very often treatment is not necessary for lipomas, it is especially in situations when they are small, silent, and do not prevent a person from his daily activities. However, if a lipoma becomes symptomatic, affects movement, causes pain, or is cosmetically bothersome, various treatment options may be considered. However, if a lipoma becomes symptomatic, affects movement, causes pain, or is cosmetically bothersome, various treatment options may be considered:
Surgical Removal (Excision):
The most typical surgical therapy for lipomas is surgical excision, in particular, if they induce symptoms or aesthetic problems. At this treatment, the abnormally grown tissue in the form of a lipoma is surgically removed under local anesthesia. The surgeon cuts over the lipoma, takes out the growth with close-by tissues if required, and sews the incision up. In most cases, surgical removal offers a permanent solution to the problem as it allows the elimination of lipoma and the prevention of its recurrence.
Liposuction:
Deep and large lipomas may be treated (Liposuction) and so may the lipomas that are found in the areas that are technically difficult and sensitive cosmetically. Liposuction, which is an operating procedure, makes a small incision near the lipoma, and a thin cannula is put in as an instrument to suction out the fatty tissue. A key benefit of liposuction over surgical excision is that it may create less scarring and have a shorter recovery period.
Steroid Injections:
In other instances, corticosteroid injections might be utilized to reduce the size or even eliminate symptoms like pain and swelling. Steroid injections are able to control the localization of the lipoma and lessen the surrounding swelling by diminishing the fatty tissue therein. Although steroid injections present a temporary solution, a higher number of injections can be needed, and the efficacy can differ between people.
Homeopathic Treatment:
Destiny bases its remedies on the specific needs of individuals by targeting the symptoms, and thus, trying to find a way of activating the body’s natural self-healing. Many people want to benefit from homeopathy. The best way to get reliable advice is by consulting qualified professionals with personalized recommendations that will suit you and open communication with primary healthcare providers is crucial. The choice to utilize homeopathic treatment should be carried out on account of the personal taste of the patient and the consultation with the health professionals.
Observation:
In cases where a lipoma is small, asymptomatic and not impacting on the life of a patient, a healthcare provider may advise to watch and see if there is a need for further intervention. Routinely following the lipoma may be needed since it helps to detect any changes that the size or symptoms might undergo or appear. If the lipoma remains stabilized without causing any problems, then the treatment may not be necessary.
In the end, the decision to treat a lipoma depends on several aspects such as the size and the location of the lipoma, the symptoms that are experienced, and the patient’s preferences. This will require the patient to consult a healthcare provider or a surgeon.
Prevention of Lipoma:
Maintaining a Healthy Weight and Lifestyle:
The combination of a balanced diet and exercise that is consistent with the accompanying weight loss plays a very pivotal role in the control of this condition. Selecting a diet with abundant nutrients, like fruits, vegetables, proteins, and also whole grains, with less quantity of processed foods and sugary drinks is a way of keeping the weight down. Following the guidelines of performing regular physical activities, such as aerobic exercises and strength training, helps in achieving overall good health and also avoiding a lipoma that occurs as an outcome of fat accumulation.
Early Detection and Timely Management:
Frequent self-skins check-ups allow for the early identification of any Asian lips mass or appearance change that could suggest that a lipoma is present. Seeking prompt medical evaluation for the lesions and growths that seem suspicious promotes accurate diagnosis and treatment. Healthcare providers can also make diagnoses and be involved in the regular check of the existing lipomas, and to protect their complications. So timely management can be done.
Healthcare Provider Guidance:
Consultations with health agencies help in gaining information that is personalized on the preventive measures of lipomas. Healthcare professionals can provide a number of recommendations that are tailored to each individual’s needs and these may incorporate diet, exercise, and also weight management strategies. Routine wellness checks and screenings with the health care providers are very suitable for those who want to maintain overall health and also the detection of any possible markers or risk factors for lipomas or other skin conditions.
Awareness and Education:
Awareness and education on lipomas as well as preventative measures is very much needed in order to ensure the skin health of the public. Discovering lipomas, their risk factors, and preventive strategies helps to shape individual skin health to empower individuals to take proactive measures. Participation in such programs/seminars like health instructions, workshops, or seminars on skin health is very valuable because it provides relevant information and resources for prevention.
Regular Skin Checks:
Regular inspection of the skin ensures that people can identify any new lumps, bumps, or skin color changes immediately. Peripheral lipomas observed at the early stage are likely to have timely medical evaluation and intervention, hence, decreasing the chances of postoperative complications and ensuring optimal management.
Healthy Lifestyle Choices:
Embodying a healthy lifestyle like abstaining from smoking, limiting alcohol intake, and handling stress levels can improve your general health and further reduce the risk of developing lipomas. Keeping in good health or well-being helps the body to prevent and relieve lipomas effectively.
Treat Lipoma With Homeopathy:
With Homeopathy treatment by Dr Care, our treatment approach is deep in understanding the personal medical history of the patient and their particular conditions. Our experienced practitioners do the needed consultations and collect the patient’s history in medical records, lifestyle, and every single symptom.
The cohesive team of doctors will sit with the patients for a series of sessions so as to dig into their medical history to understand the underlying cause of their lipoma development. This personalized approach gives the ability to develop treatment plans that address the factors that lead to the growth of lipomas in each individual case.
Homeopathic medications are prescribed by our doctors who identify the exact triggers and the body imbalances and match the remedies to each patient’s constitution and the symptoms. The remedies are precisely picked to activate the body’s innate healing capabilities and cause the recession or complete regression of lipomas.
At Dr Care Homeopathy focuses on personalized care and comprehensive analysis to provide the best available gentle treatment for lipomas in a holistic manner. Our physicians spare no effort to comprehend each patient’s particular requirements and issues, which helps them reach their full potential of health and delight.